
EO gold standard for endoscope reprocessing
Complex Devices that cannot be dependably disinfected:
Duodenoscopes are a type of upper gastrointestinal endoscope used during endoscopic retrograde cholangiopancreatography, or ERCP, to diagnose and treat disorders of the bile and pancreatic ducts.
Urological endoscopes are used for viewing and accessing the urinary tract.
Bronchoscopes may be used to examine, diagnose and treat disorders and diseases of the throat, larynx, trachea, and lower airways.
Which device will be next?
Complex device reprocessing, superbugs and EO
According to the U.S. Centers for Disease Control (CDC), on any given day one in 31 hospital patients has at least one healthcare-associated infection.1 More healthcare-associated outbreaks have been linked to flexible endoscopes than to any other type of medical device.2
The mortality rates for patients infected with certain multidrug-resistant organisms (MDRO) can be as high as 50%.4,3
To date, ethylene oxide (EO or EtO) sterilization has proven to be the most effective tool in combating MDRO.
Setting the stage
“Superbugs” are strains of bacteria, viruses, parasites and fungi that are resistant to most antibiotics and other medications commonly used to treat the infections they cause. These classes of antibiotics can include carbapenems – which are “last resort” antibiotics used to treat many types of serious infections caused by multidrug-resistant bacteria.3
Carbapenem-resistant Enterobacteriaceae – or CRE – are a particularly pernicious family of gram-negative bacteria resistant to these antibiotics. CRE and related superbugs have become a global public health scourge. The mortality rates for patients infected with CRE and certain other superbugs, particularly bloodstream infections, can be as high as 50% – or higher, in some patient subgroups.4,3
In February 2015, the U.S. Food and Drug Association (FDA) acknowledged for the first time, that duodenoscopes could remain persistently contaminated with life-threatening superbugs and related multidrug-resistant organisms.5 Examples of these potentially deadly microorganisms include CRE and carbapenem-resistant Pseudomonas aeruginosa.
During its subsequent review of several duodenoscope-related outbreaks, the FDA found that many of the superbug infections occurred despite staffers cleaning and disinfecting the duodenoscope in accordance with manufacturer’s instructions.
According to the FDA, the complex physical design of duodenoscopes “may impede effective reprocessing,” ominously stressing that “meticulously cleaning duodenoscopes prior to high-level disinfection should reduce the risk of transmitting infection but may not entirely eliminate it.”5
This was a watershed finding because, previously, virtually every infection associated with a contaminated duodenoscope, or other type of flexible endoscope, had been attributed to a reprocessing breach – more specifically, to failure to clean and disinfect the device as instructed in its labeling. Reprocessing a flexible endoscope as prescribed by the manufacturer had always prevented cross-infection (with few exceptions) until that time first recognized in 2015.5
To combat the infection risk, enhance reprocessing and improve the safety of duodenoscopes, FDA advised healthcare facilities, in a safety communication published a few months later, in August 2015, to consider implementing one or more of four enhanced, or “supplemental,” measures, which included ethylene oxide sterilization.6
Drawing a distinction between disinfection and sterilization, FDA stated in August 2015 that “duodenoscopes should be subjected to high-level disinfection following manual cleaning after each use. When possible and practical, duodenoscopes should be sterilized due to the greater margin of safety provided by sterilization.”6
(Deadly) Alphabet Soup
MDRO: Multidrug-resistant microorganisms. Strains of bacteria, viruses, parasites and fungi that are resistant to most antibiotics and other medications commonly used to treat the infections they cause. Also known as superbugs.
CRE: Carbapenem-resistant Enterobacteriaceae, a particularly pernicious superbug.
HAI: Hospital acquired infection or nosocomial infection. Most superbugs are acquired in a healthcare setting.
Common Superbugs
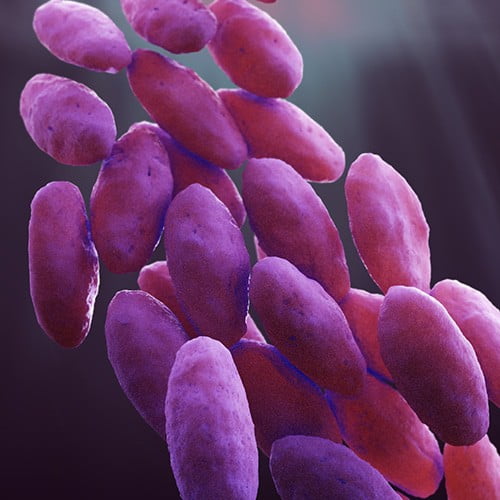
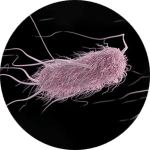
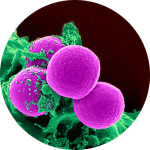
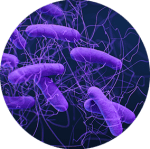
Indeed, subsequent field surveillance later confirmed ethylene oxide (EO) sterilization was the most effective of the supplemental measures, and validation studies showed that it was the only measure that assures the complete inactivation of highly resistant microorganisms.7
A rising infection risk?
Some data suggest that the incidence of a duodenoscope transmitting microorganisms, including CRE and other potentially deadly superbugs, during ERCP decreased, at least for a time, following the FDA’s alerts in 2015 informing healthcare facilities and device manufactures about this public health risk.8
However, reports submitted to the FDA’s adverse event database for medical devices, or “MAUDE,” since 2015 indicate that, while the number of FDA reports linking a duodenoscope to an infection apparently decreased in 2016 and even more so in 2017 compared to the relatively high number of cases reported to the FDA in 2015.8 But 2018 reversed the trend and in 2019 the FDA received twice as many reports.
Ratcheting up the stakes, a report published in 2019 linked a duodenoscope to the possible transmission of a superbug carrying the mcr-1 gene, which can confer colistin antibiotic-resistance to the microorganism.9 Like carbapenems, colistin may be used as a “last line of defense” for treating some types of multidrug-resistant infections. Notably, some colistin-resistant infections may be untreatable.
Several factors may explain these troubling trends, but one clear point warrants particular attention: The risk of infection associated with use of a duodenoscope remains a concern today.
Indeed, according to the CDC, more healthcare-associated outbreaks have been linked to flexible endoscopes than to any other type of medical device.
CDC
FDA published alerts in 2019 and 2020 recommending that healthcare facilities and manufacturers “begin transitioning to duodenoscopes with disposable components” and, in the later alert, stressed “sterilization, particularly terminal (e.g., gas) sterilization, provides a greater margin of safety than high level disinfection.”10
Andersen solves problem
In 2015, Andersen Sterilizers had a duodenoscope clearance underway with the FDA. Because of the CRE outbreak, Andersen was forced to withdraw its claim. At the time, the agency wasn’t sure of the source of infections or how to test these complicated instruments post-sterilization.
Andersen spent the next two years negotiating testing protocols with the FDA. During this time duodenoscopes were redefined as a “collection of instruments.” A new validation and simulated use testing protocol was chosen: The duodenoscope is inoculated at seven of the hardest-to-reach sites in the scope with 106 bacterial spores.
This is a significantly higher bar than any previous FDA requirement. Andersen is very proud to have achieved it.
Andersen validated duodenoscopes from all three major endoscope manufacturers and a colonoscope with an 11’6″ channel x 1.2mm.
Bronchoscopes and urological endoscopes pose a risk, too
Early in 2021, FDA acknowledged that other types of flexible endoscopes also remain a concern and may pose a risk of infecting patients with superbugs and related multidrug-resistant organisms.
In April, FDA issued a letter to raise awareness among healthcare providers “about the risk of infections associated with reprocessed urological endoscopes, including cystoscopes, ureteroscopes, and cystourethroscopes.”11
FDA wrote this April letter after acknowledging receipt of “over 450” medical device reports describing “patient infections post procedure or other possible contamination issues associated with reprocessing these devices.”11
Similar to the circumstances surrounding the infections linked to “reprocessed” duodenoscopes, FDA concluded in the letter that both the reprocessing instructions and designs of urological endoscopes could be factors contributing to these reported cases of infection and device contamination. Similar to earlier alerts, the FDA advises facilities to follow IFUs, maintain their devices correctly and gives two reprocessing choices – one of which includes sterilization.11
Two months later in June, FDA published a safety communication alerting the public to the risk of a third type of flexible endoscope ― reprocessed bronchoscopes ― similarly infecting patients with multidrug-resistant bacteria, again including CRE.12 The FDA’s notice provides updated advice that supplements the FDA’s earlier (and now outdated) alert, published in September 2015, also discussing infections linked to reprocessed (flexible) bronchoscopes.13
This June alert focusing on bronchoscopes provided two new recommendations that were not discussed in the earlier 2015 communication: first, that healthcare facilities “consider using sterilization instead of high-level disinfection when feasible because sterilization has a greater safety margin than high-level disinfection.” Otherwise, if “sterilization is not available,” then high-level disinfection of bronchoscopes should be performed.12
Second, the FDA’s June alert recommends that healthcare facilities “not use damaged devices or those that have failed a leak test, as they could be a potential source of contamination.” Examples of endoscope damage include loose parts; damaged channel walls; and other signs of wear or damage.12
Soapbox
The June 2021 FDA alert also says, “Consider using a single-use bronchoscope in situations where there is an increased risk of spreading infection (for example, multidrug-resistant microorganisms, immunocompromised patients, or patients with prion disease) or when there is no support for immediate reprocessing of the bronchoscope.”
The FDA is advising the use of a type of endoscope (reusable, single-use) based on the immuno-status of the patient. This can introduce two standards of care, which is problematic. Sterilizing with EO resolves this issue.
Moreover, is the FDA stating that in situations where there is no perceived increased risk of spreading infection, that single-use bronchoscopes not necessarily be considered? This is confusing … Who is to decide whether there is an increased risk, and what defines “increased,” other than the very broad definition in the quote? What about undetected infections?
Growing support
The American Society for Gastrointestinal Endoscopy updated their “Multisociety guideline on reprocessing flexible GI endoscopes and accessories” in 2021 to state, “The use of EtO sterilization on duodenoscopes during infectious outbreaks has been associated with terminating these outbreaks and such a modality should be considered in selected settings and patient populations.”14
The Multisociety guideline goes on to reference the work of Larry Muscarella, a frequent collaborator here at Andersen, “EtO sterilization of duodenoscopes can be an effective tool in some clinical situations, specifically when there are infectious outbreaks observed among patients who have undergone ERCP. A systematic review by Muscarella examined all reported carbapenem-resistant Enterobacteriaceae–and multidrug-resistant organisms–related infections in the United States and Europe attributed to duodenoscope exposure and assessed the adequacy of reprocessing in these outbreaks.
Factors such as endoscope design, lapses in reprocessing guidelines, damage to the endoscope, or a lack of servicing, maintenance, and repair of the endoscope were hypothesized to be contributors to these outbreaks. In this review, 6 of 17 studies implemented EtO sterilization as an intervention during infectious outbreaks; in at least 3 and possibly 6 studies this intervention yielded an absence of culture positivity from duodenoscopes at all sites, thereby stopping the outbreaks. Similar data exist for EtO sterilization ceasing outbreaks attributed to bronchoscopes. Therefore, the implementation of EtO sterilization appears to be an effective tool for terminating carbapenem-resistant Enterobacteriaceae and multidrug-resistant organism outbreaks associated with duodenoscopes.”
Soapbox
The Multisociety guideline goes on to say, “However, sterilization technology is costly, inefficient, and associated with potential toxicity to reprocessing personnel and surrounding communities; additionally, there are concerns about endoscope performance and durability, and such technology is not widely available.”
In its 4 Supplemental Measures document (2015) FDA says, “Implementing EtO gas sterilization is costly and the process may not be readily available in or accessible to all health care facilities. EtO may affect the material and mechanical properties of the duodenoscope.”
It seems both companies are describing processes from a bygone era – the old 50 lb tank systems of old, perhaps. In any case, they describe precisely what an Andersen sterilizer is not. Our sterilizers are affordable, incredibly efficient due to our exclusive technology, present very comparable risk to operators (see chart below) and the surrounding community to other sterilization/disinfection methods, are so incredibly gentle we say the process is “zero damage” and, of course, they’re readily available.
Hospitals fell out of love with EO
Ethylene oxide was the dominant hospital sterilant from the late 1960s until the late 1990s, when newer modalities like hydrogen peroxide began gaining ground.
Those now-obsolete EO systems, a staple of hospital life in the 1980s, quite simply deserved to be supplanted. They were fed by 50-pound tanks of EO which had to be stored in specially ventilated rooms. They required external air compressors, water lines and a second room to protect operators from gas exposure. Emission abators worked by burning excess EO and, since the gas is highly flammable, the whole system occasionally exploded.
It is unfortunate, however, that the indisputable drawbacks of early EO systems have caused many to overlook their modern progeny – which have mitigated these drawbacks and, again, offer an indispensable tool in the fight against deadly MDRO.
Modality in-fighting
Some competing modalities have waged a damaging campaign against ethylene oxide for nearly half a century. The sustained onslaught has successfully convinced consumers that EO is far more toxic and far more dangerous than these competing modalities.
This is simply untrue. All chemicals capable of terminal sterilization deserve to be treated with the same level of care and are rated very similarly by governing agencies.
| Ethylene Oxide | Hydrogen Peroxide | Peracetic Acid | Glutaraldehyde | |
|---|---|---|---|---|
| OSHA 8hr/15min PEL: Permissible Exposure Limits | 1 ppm / 5 ppm | 1 ppm / – | – / – | – / – |
| ACGIH 8hr/15min TLV: Threshold Limit Values | 1 ppm / – | 1 ppm / – | – / 0.4 ppm | 0.05 ppm / – |
| NIOSH 8hr/10min REL: Recommended Exposure Limit | <0.1 ppm / 5 ppm | 1 ppm / – | – / – | 0.2 ppm / – |
| NIOSH IDLH: Immediately Dangerous to Life or Health | 800 ppm | 75 ppm | 0.55 ppm (proposed) | – / – |
| HSE 8hr/15min WEL: Workplace Exposure Limits | 1 ppm / – | 1 ppm / 2 ppm | – / – | 0.05 ppm / 0.05 ppm |
| Cancer Status | IARC: Carcinogenic to Humans ACGIH: Suspected Human Carcinogen | IARC: Not Classifiable as to Carcinogenicity in Humans ACGIH: Confirmed Animal Carcinogen with Unknown Relevance to Humans | ACGIH: Not Classifiable as a Human Carcinogen | – / – |
| Odor Threshold | 400 to 700 ppm | Almost no odor | 50 ppm | 0.04 ppm |
| CAMEO Datasheet | Ethylene Oxide | Hydrogen Peroxide | Peracetic Acid | Glutaraldehyde |
| Downsides | Cycle times (Andersen: 3.5 – 26 hours including standard aeration) | Acquisition, labor, operating and service costs, reliability issues, struggles to sterilize long lumens, pulls a deep vacuum that can damage delicate items, corrosive | Immersible instruments only, makes plastic brittle, corrodes metal, can only process one scope or a small number of instruments per cycle | |
| NOT compatible with | Food, drugs or liquids | Cloth, liquids, paper, powders, anodized aluminum and anything containing cellulose | Aluminium, carbon steel, some cross-linked polyethylene and metal alloys containing copper |
Ethylene oxide is rated as having comparable risk as other common sterilants. EO and hydrogen peroxide (H2O2 or “plasma”) have the same Permissible Exposure Limit (PEL) of 1 ppm and the proposed PEL for peracetic acid (PAA) is even lower (worse).
The U.S. National Institute of Occupational Safety and Health (NIOSH) defines Immediately Dangerous to Life or Health (IDLH), as exposure to atmospheres “likely to cause death or immediate or delayed permanent adverse health effects or prevent escape from such an environment.”15 The IDLH for EO (800 ppm) is ten times higher than for H2O2 (75 ppm) – in this instance, a higher number represents lower risk.
For PAA, many are surprised to learn that NIOSH is considering a proposed IDLH value that is lower still. Keep in mind that PAA is a combination of H2O2 and acetic acid – both of which have limits set from all agencies above. More stringent guidelines are under consideration and likely coming.
EO: Gentle, mighty & compatible
EO was chosen as the dominant method of hospital sterilization for good reason. Both then and now it offers terminal sterility (SAL 10-6) with an incredibly gentle cycle; low temperature, no steam, no deep vacuum, no oxidation, no dulling, no damage.
The modality can be used with nearly any material – including plastic, fabric, cellulose, rubber – as well as with delicate, moisture- or heat-sensitive devices. Ethylene oxide can sterilize through mated or threaded metal surfaces. It will permeate through sealed plastic, Tyvek® and other wrapping – leaving the objects inside sterilized and protected from contamination (providing a sterile shelf life).
So, what changed?
Game changer
The major difference between the obsolete tank-based systems and modern ones is the dose of EO used in each cycle. Modern manufacturers of EO sterilizers for the healthcare market use from 170 grams all the way down to Andersen Sterilizers’ microdose, just 17.6 grams.
Using this microdose of EO packaged in a single-use cartridge mitigates many former safety issues all on its own. Andersen sterilizer systems require no water line and no exterior air compressor.
Instead of being catalytic (works by burning EO) our optional emission abators are cationic (works by capturing EO in a resin bed which turns into biodegradable organic compounds). There is no flame or spark source that could propagate back to the sterilizer and create an explosion.
Andersen’s proprietary technology, Ethylene Oxide – Flexible Chamber Technology (EO-FCT), levels up “modern.” In Andersen’s systems, the sterilization bag acts as the sterilizer while the cabinet acts as a ventilation hood – to keep air moving from the front to the back and then to the outside. This chamber-within-a-chamber redundancy mitigates the need for a second room to protect the user from exposure.
EO-FCT also allows Andersen to use 90% less gas than any system on the market. Excess air is removed from the sterilization bag before the cartridge is activated so the gas has the smallest possible area to move in. It has nowhere else to go but directly into the items to be sterilized.
EO-FCT is exclusive, patented and exhaustively tested. Andersen Sterilizers has several U.S. Food and Drug Administration (FDA) Clearances on the process.
Conclusions
The risk of superbug infections associated with reprocessed duodenoscopes, bronchoscopes and urological endoscopes, among other types of flexible endoscopes, is a growing concern today, warranting attention and risk mitigation.
Failure to properly reprocess a flexible endoscope has been directly linked to deadly infections of CRE, carbapenem-resistant P. aeruginosa and related superbugs.16 The mortality rates of superbug infections can be as high as 50%, or higher.17 Cleaning and disinfecting the endoscope correctly, in accordance with manufacturer instructions, significantly reduces the infection risk, but may not entirely eliminate it, according to the FDA. 5,13
The FDA has repeatedly recommended ethylene oxide gas sterilization over high-level disinfection for reprocessing endoscopes because of its “greater safety margin.”12 Numerous studies have documented that EO sterilization of endoscopes during infectious outbreaks has been associated with terminating these outbreaks.7
Andersen holds the ONLY FDA clearance for terminal sterilization for duodenoscopes and colonoscopes, with a maximum lumen length of 3530 mm (11.6 feet) and minimum lumen diameter of 1.2 mm (the thickness of a Blu-Ray, less than the height of a dime).
We also hold FDA-clearances for urological endoscopes and bronchoscopes, including: bronchovideoscopes, cystoscopes, ureteroscopes, choledocoscopes, gastrovideoscopes and gastrointestinal videoscopes.
Savvy CPD managers are taking a second look at ethylene oxide sterilization. Long gone are the tank systems of old. The serious and growing threat of MDRO, comparable toxicity and far superior efficacy in the fight against them, as well as technological advances in the modality have once again earned a place for the modern EO sterilizer in a well-run central processing department.
recap
- EO is the FDA-recommended method for reprocessing flexible endoscopes because of its greater margin of safety
- Andersen holds recent (post-2015) FDA-clearances for flexible endoscopes in all of troublesome categories. In some cases, we hold the only clearance.
- We hold clearances for chemical and biological indicators and packaging that maintains sterility of endoscopes for 3-6 months after reprocessing.
- Our sterilizers are tabletop (two larger models available). They are easy to install and use – with free training for the life of your sterilizer. An Andersen Sterilizer is a seamless addition to your practice.
- For critical instruments and compromised patients an Andersen sterilizer is cheap insurance.
Is it time to protect your patients and safeguard your business?
